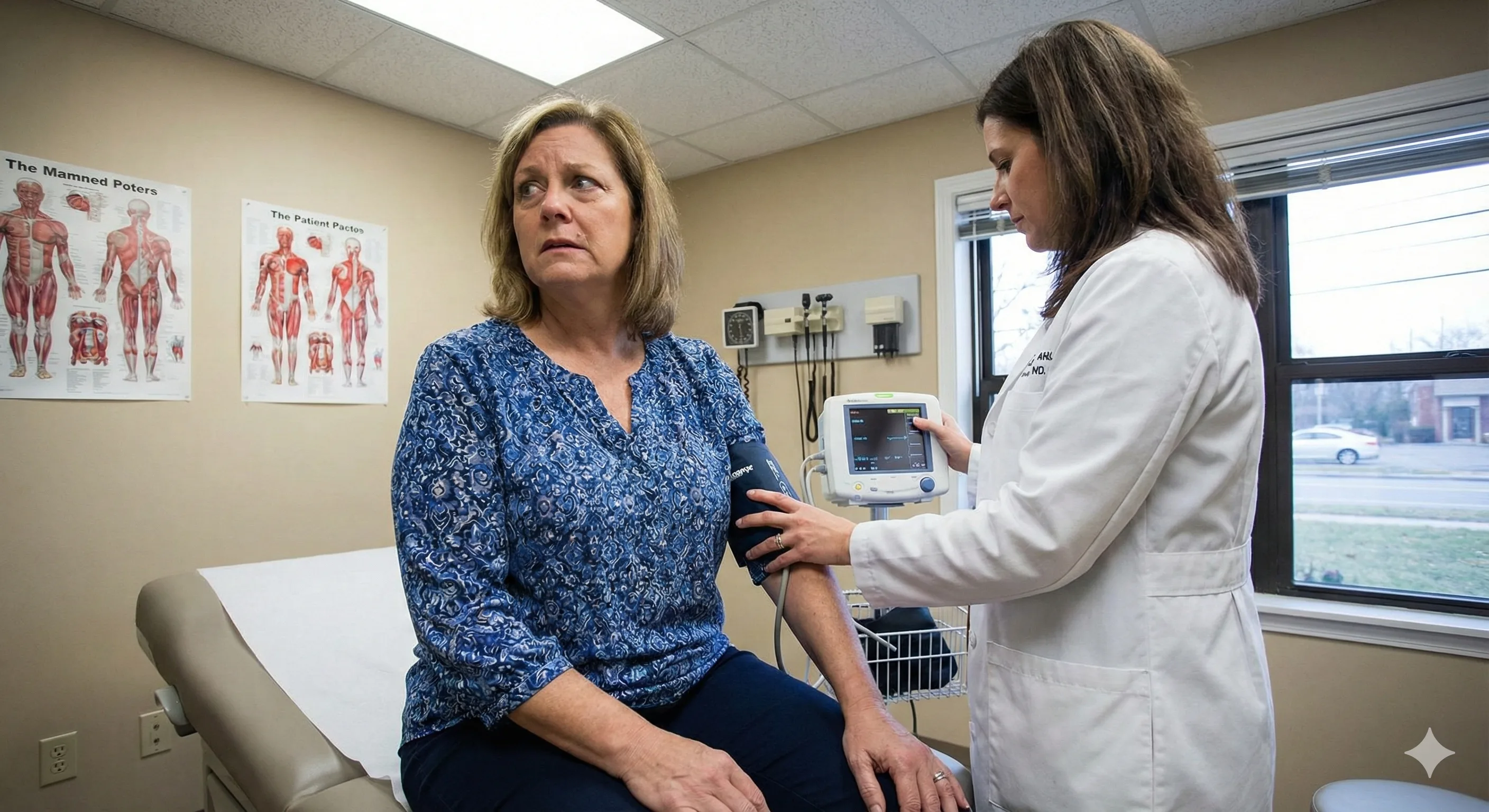
If you're living with high blood pressure, you might know this feeling: at home, your numbers are "okay." But the moment you walk into the clinic, your blood pressure suddenly jumps. That spike in the doctor's office has a name: white coat hypertension (also called white coat syndrome).
It happens when your blood pressure rises in medical settings due to anxiety or stress. You're not imagining it—it's a real physiological response that affects up to 30% of people who get their blood pressure checked.
What Causes White Coat Hypertension?
The underlying cause is your body's stress response. When you're anxious—even if you don't feel particularly nervous—your sympathetic nervous system kicks in. This releases stress hormones like adrenaline and cortisol, which cause your heart to beat faster and your blood vessels to constrict.
Common triggers include:
- Anticipation of bad news or a diagnosis
- Discomfort with medical procedures
- Past negative experiences at the doctor
- General anxiety about health
- Feeling rushed during the appointment
Is White Coat Hypertension Dangerous?
While a temporary spike isn't immediately dangerous, research suggests that people with white coat hypertension may be at higher risk of developing sustained hypertension over time. A 2019 meta-analysis in the Annals of Internal Medicine found that untreated white coat hypertension was associated with a 36% higher risk of cardiovascular events.
The Bottom Line
How to Beat White Coat Syndrome
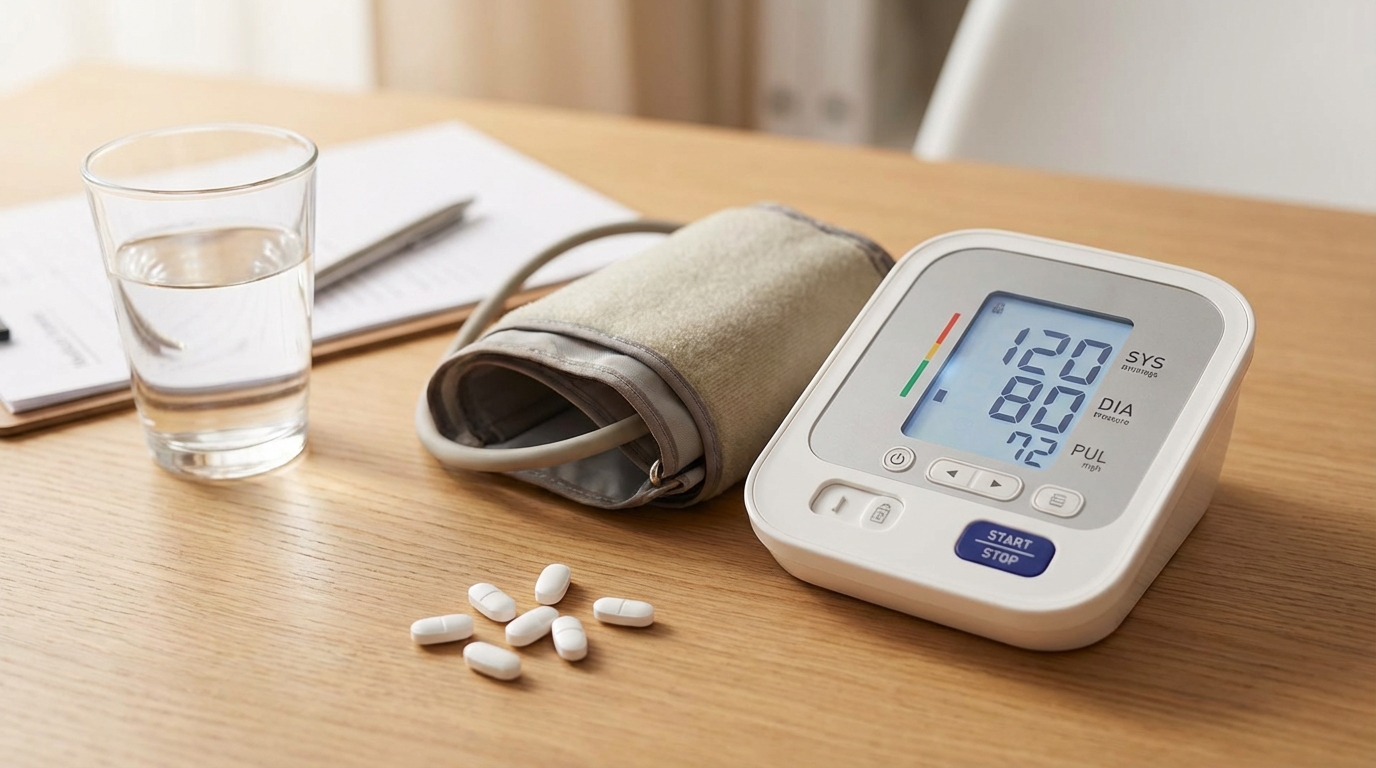
1. Monitor Your Blood Pressure at Home
The most effective way to manage white coat hypertension is to track your blood pressure at home. Use a validated monitor and measure at the same times each day—typically morning and evening. This gives you and your doctor accurate data about your true blood pressure levels. Keep a blood pressure log to track all your readings in one place.
2. Practice Relaxation Before Your Appointment
Arrive at your appointment 10-15 minutes early so you're not rushed. Practice deep breathing: inhale for 4 seconds, hold for 4 seconds, exhale for 4 seconds. This activates your parasympathetic nervous system and helps lower your heart rate.
3. Talk to Your Healthcare Provider
Let your doctor know you experience white coat hypertension. They may take multiple readings, wait a few minutes before measuring, or rely more heavily on your home readings. Some clinics also offer ambulatory blood pressure monitoring, which tracks your BP over 24 hours. To understand the different measurement methods, read about how blood pressure is measured.
4. Focus on Lifestyle Factors
Reducing overall stress and improving cardiovascular health can help minimize white coat hypertension effects:
- Regular exercise (150 minutes of moderate activity per week)
- Reducing sodium intake to less than 2,300 mg/day
- Limiting alcohol and caffeine
- Getting 7-9 hours of quality sleep
- Practicing stress management techniques like meditation
5. Bring Your Home Data to Appointments
When you share a week or two of home readings with your doctor, they get a much clearer picture of your cardiovascular health. Apps like Cardilog make it easy to track readings, visualize trends, and generate professional PDF reports that you can share with your healthcare provider.
Treatment Options for White Coat Hypertension
Not everyone with white coat hypertension needs medication. Treatment depends on whether your blood pressure is elevated only in clinical settings or also at home, and whether you have other cardiovascular risk factors.
When Medication May Be Recommended
Doctors typically consider medication for white coat hypertension when home or ambulatory readings also show sustained elevations—particularly when systolic pressure is consistently above 140/90 mmHg or when other risk factors like diabetes, kidney disease, or a history of cardiovascular events are present.
Commonly prescribed medications include:
- Beta-blockers (e.g., propranolol): These reduce the physical symptoms of the stress response by slowing heart rate and lowering the force of heart contractions. Propranolol is often preferred because it also reduces anxiety-related symptoms like trembling and rapid heartbeat.
- ACE inhibitors (e.g., lisinopril, ramipril): These relax blood vessels by blocking the production of angiotensin II, a hormone that constricts arteries. They are a common first-line treatment when home readings confirm sustained hypertension.
- Calcium channel blockers (e.g., amlodipine): These relax the muscles of blood vessel walls and may be prescribed when other medications are not suitable or when additional blood pressure lowering is needed.
Your doctor will choose a medication based on your overall health profile, existing conditions, and how you respond to treatment. Never start or stop blood pressure medication without consulting your healthcare provider.
Non-Pharmacological Approaches
For many people with white coat hypertension, non-drug approaches can be highly effective— especially when office-only elevations are the primary concern:
- Cognitive behavioral therapy (CBT): Working with a therapist to identify and reframe anxiety triggers related to medical settings. Studies show CBT can reduce white coat hypertension by addressing the root psychological causes.
- Biofeedback: Using real-time data (heart rate, muscle tension) to learn how to consciously control your stress response. Some practitioners use biofeedback specifically for blood pressure management.
- Meditation and mindfulness apps: Regular meditation practice has been shown to reduce anxiety and lower resting blood pressure. Even 10 minutes a day can make a difference over time.
- Regular home monitoring: Tracking your blood pressure at home with a blood pressure log reduces anxiety by giving you confidence in your actual numbers. When you bring documented home data to appointments, you feel more in control.
Clinical Guidelines
Both the American Heart Association (AHA) and the European Society of Cardiology (ESC) have published guidelines on managing white coat hypertension:
- The AHA recommends confirming white coat hypertension with out-of-office measurements (home or ambulatory monitoring) before initiating treatment.
- The ESC guidelines suggest that white coat hypertension without target organ damage may be managed with lifestyle modifications and regular monitoring rather than immediate medication.
- Both guidelines emphasize that 24-hour ambulatory blood pressure monitoring (ABPM) is the gold standard for distinguishing white coat hypertension from sustained hypertension.
- Annual follow-up with home monitoring is recommended, as up to 40% of people with white coat hypertension may develop sustained hypertension over 5-10 years.
Important
White Coat Hypertension vs Masked Hypertension
White coat hypertension and masked hypertension are opposite conditions, and understanding the difference is important. With white coat hypertension, your blood pressure is high in the clinic but normal at home. With masked hypertension, your blood pressure appears normal in the clinic but is actually elevated at home and during daily life.
Masked hypertension is particularly concerning because it often goes undetected during routine office visits. Studies suggest it carries a cardiovascular risk similar to—or even higher than—sustained hypertension, precisely because it is less likely to be diagnosed and treated.
This is another reason why home monitoring is essential. Whether you experience white coat hypertension or suspect masked hypertension, regularly checking your blood pressure at home and sharing the data with your doctor ensures that neither condition goes unnoticed. Use a blood pressure chart to track where your home readings fall relative to clinical guidelines.
When to Seek Treatment
If your home readings are consistently elevated (above 130/80 mmHg), don't assume it's just white coat hypertension. Work with your doctor to determine whether lifestyle changes or medication might be appropriate. The goal is to keep your blood pressure in a healthy range—wherever you are.